|
1/20/2023 0 Comments U.s.counties in jmp graph builder  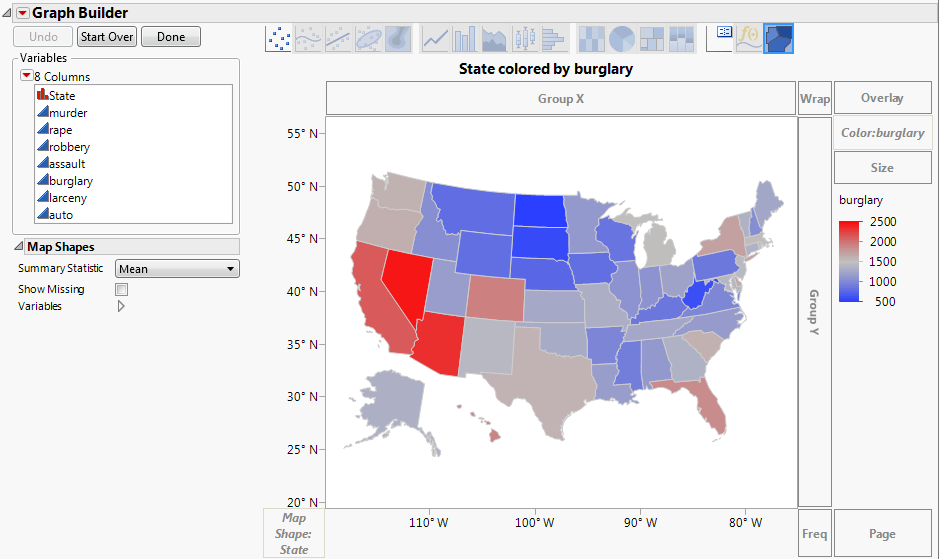
A complete list of demographic and socioeconomic variables with data available is included in Table 1. Most of the variables with limited data availability were race-specific variables for minority populations (e.g., number of firearm fatalities-Black, motor vehicle crash deaths-Hispanic), so these could not be included in the analysis. A data completeness threshold of 70% was set and redundant variables were filtered out, resulting in 44 out of a total of 131 variables from the 2020 County Health Rankings. However, it remains unclear whether disparities in vaccine rollout and associated COVID-19 infection rate fluctuations have been driven by some specific socioeconomic and population health factors.ĭemographic and socioeconomic data for each county were obtained from the 2020 County Health Rankings resource provided by the County Health Rankings & Roadmaps program at the University of Wisconsin Population Health Institute. Outside of the US, researchers have found significant correlations between socioeconomic status and vaccination acceptance rates in Israel, and vaccine hesitancy is a worldwide issue. In addition, another recent analysis of 580 US counties found that the change in COVID-19 incidence from 1 December 2020 to 1 March 2021 is significantly correlated with cumulative vaccination rate through 1 March 2021. This study did not, however, assess the interplay between these factors and new COVID-19 incidence rates. A recent study by the CDC showed that vaccine coverage is lower in counties with high social vulnerability based upon socioeconomic indicators (poverty, unemployment, low income, no high school diploma). Social determinants of health (SDoH) and aspects of an individual’s life that occur “outside of the four walls of healthcare” have a tremendous impact on actual health status. However, this rapid vaccine rollout has not benefited all Americans equally, and the vaccination rate in some marginalized communities has lagged significantly behind the average. 
The COVID-19 vaccine rollout in the United States has been among one of the fastest in the world. This study shows that socioeconomic factors are strongly correlated to both COVID-19 vaccination rates and incidence rates, underscoring the need to improve COVID-19 vaccination campaigns in marginalized communities. In addition, severe housing problems and high housing costs were strongly correlated with increased COVID-19 incidence (Spearman correlations: 0.335, 0.314, p-values: <0.001, <0.001). These correlation analyses demonstrated that counties with high levels of uninsured individuals have significantly lower COVID-19 vaccination rates (Spearman correlation: −0.460, p-value: <0.001). This correlation analysis was also performed using multivariate linear regression to adjust for age as a potential confounding variable. In particular, using data from 3142 US counties with over 328 million individuals, correlations were computed between cumulative vaccination rate and change in COVID-19 incidence from 1 December 2020 to 6 June 2021, with 44 different demographic, environmental, and socioeconomic factors. Here, the impact of demographic, socioeconomic, and environmental factors on county-level vaccination rates and COVID-19 incidence changes is assessed. Equitable vaccination distribution is a priority for outcompeting the transmission of COVID-19.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
